A new clinical trial has launched at Royal Papworth Hospital in Cambridge which is using ethanol (an alcohol) detected in exhaled breath as a potential tool to diagnose lung cancer earlier.
The EVOLUTION trial is recruiting patients who definitely have lung cancer and healthy volunteers who definitely do not.
A liquid solution containing a metabolic probe is administered intravenously, travels around the body and when it reacts with a lung tumour causes the release of a type of ethanol (D5).
After a set amount of time, patients breathe at regular intervals into a special mask which collects the ethanol which is then analysed in the laboratory.
The eVOC probe (Exogenous Volatile Organic Compound) has been developed by Cambridge company Owlstone Medical, who have collaborated with Royal Papworth Hospital’s thoracic oncology research team for previous breath biopsy studies.
Professor Robert Rintoul, Lead Clinician for Cancer at Royal Papworth Hospital, said: “We know from previous work that there is an enzyme around the tumour cells called glucuronidase. The glucuronidase in the lung cancer processes the eVOC probe releasing the ethanol which can be detected in breath.
“If you have got lung cancer we should see an ethanol signal in the breath; if you have not got lung cancer then there is nothing to process and so there should not be any ethanol signal present.
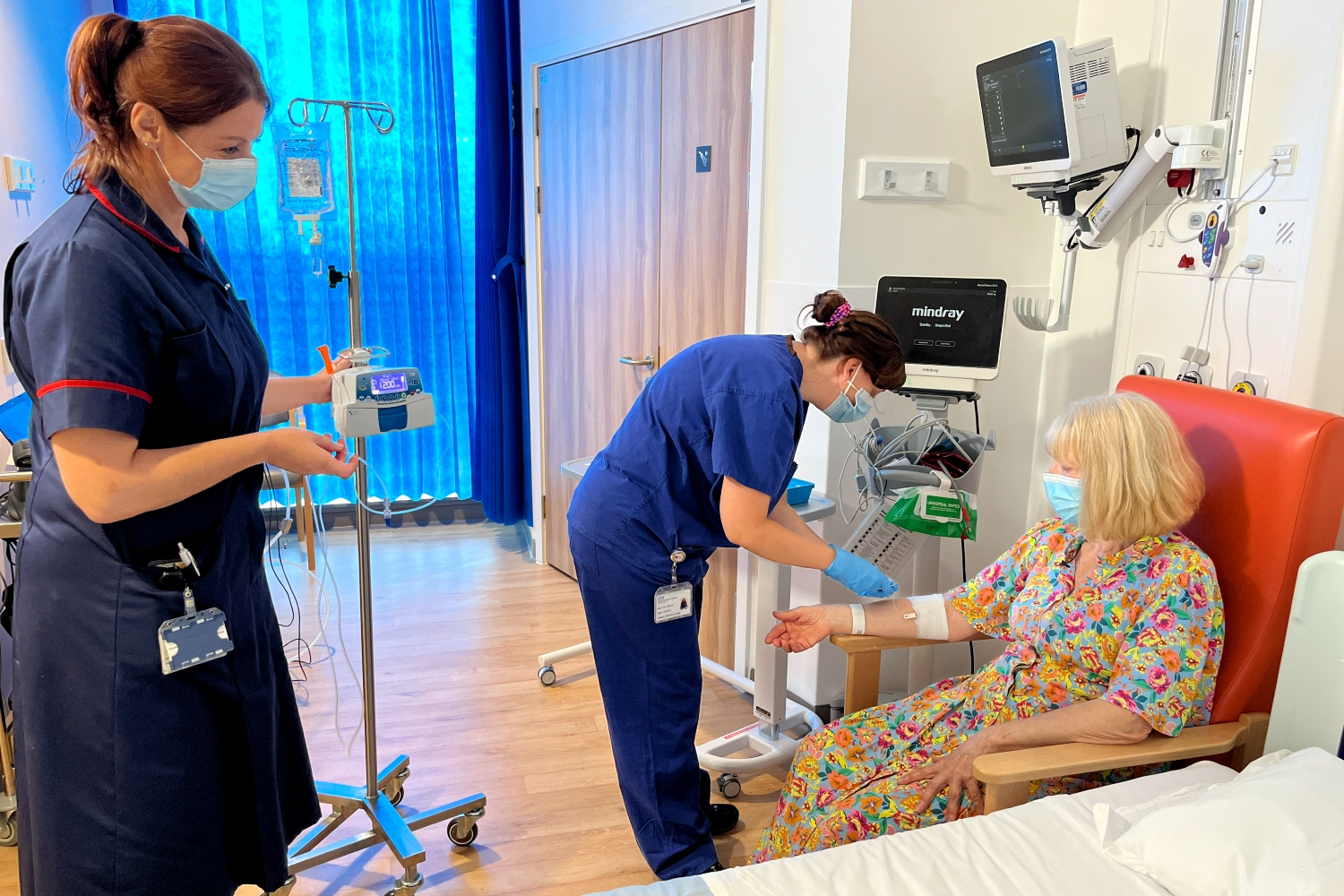
The eVOC probe is administered into the body via a vein
“At the moment it requires a lot of equipment, an intravenous injection of the probe and patients have to breath into the mask a few times over the course of a few hours.
“We hope that if this ‘proof of principle’ trial can demonstrate a difference in ethanol levels between people who do and do not have lung cancer, we can then simplify the process.
“Ideally, we would like to develop a probe that can be inhaled rather than injected and a much simpler breath collection device. If so, we might be able to use it in the GP surgery or even at home as a lung cancer screening tool for at-risk patients.
“This is a very exciting beginning. It opens a new, innovative avenue for detecting lung cancer. If we can develop this further and roll this out it will save lives.”
Billy Boyle, Co-Founder and CEO at Owlstone Medical: “Breath Biopsy has proven to be extremely effective at detecting VOCs in the breath, and we are pleased to be working with Royal Papworth Hospital as we look to apply it towards the incredibly important area of detecting early-stage lung cancer in patients.”
Lung cancer is the third most common cancer in the UK, with roughly 48,000 people diagnosed each year.
It is the biggest cancer killer with only 16% of lung cancer patients in the UK surviving five or more years.
This is mainly because most people do not develop any symptoms – such as a persistent cough, coughing up blood, regular chest infections and weight loss - until the disease is more advanced and therefore harder to treat and cure.
“Just a quarter of lung cancers are detected at an early stage when treatment is more likely to be successful,” explained Professor Rintoul.
“Many of these cases are picked up by chance because they had x-rays or scans for other reasons.
“A decade ago lung cancer survival for five or more years was 7-8%. Now it is 16%. By 2025 it is hoped that 25% of all people diagnosed with lung cancer survive.
“To do this, we need to do more to find lung cancer at the earliest stages. Through driving early detection up and up, survival rates should follow. Possible screening tools as CT scanning and this breath biopsy equipment is therefore vital.”
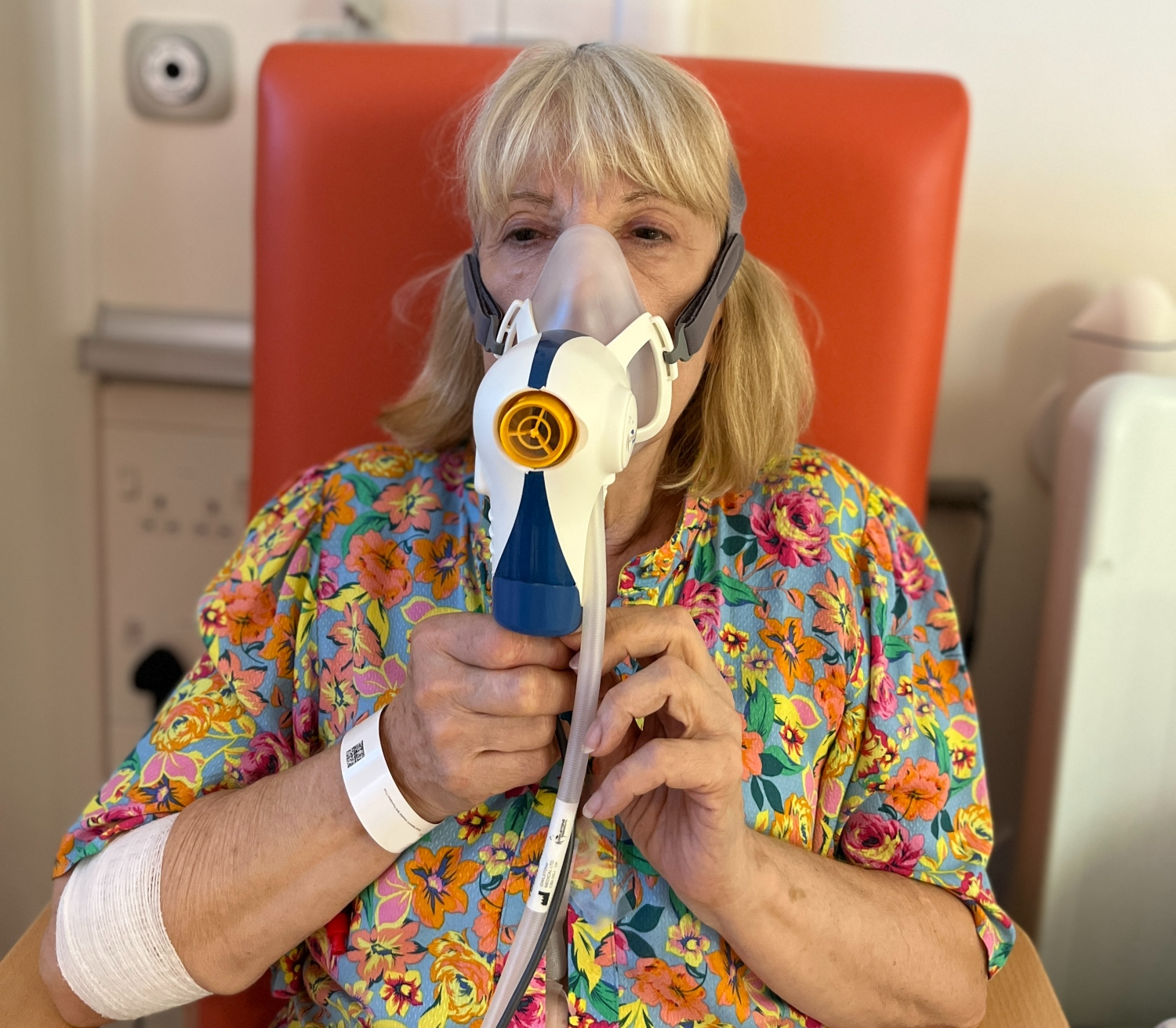
Wendy is one of the first patients recruited to the EVOLUTION trial
One of the first patients recruited to the trial is Wendy, 70, from Melbourn in South Cambridgeshire.
Wendy has early-stage lung cancer, which was found during a hospital CT scan on her back ahead of spinal surgery.
She went straight to her GP and was placed onto the cancer pathway: a PET scan at Addenbrooke’s Hospital followed before a biopsy and consultation at Royal Papworth Hospital where lung cancer was diagnosed.
“My grandmother, mother and father all died of lung cancer, and although I stopped smoking 16 years ago I was a heavy smoker for a number of years, so I always knew I would be at risk,” Wendy said.
“I am very lucky that my cancer is early stage and treatable with surgery. My parents were not so lucky – they both died a few months after being diagnosed.
“The mask is really comfortable, the nurses are so good and it’s been a relaxing, comfortable experience.
“Research like this is very important. So many people would benefit from this early detection test which is amazing. It is why I was so keen to sign up to research and would encourage all patients to do the same.”
The trial (Safety and Dose Ranging Study for OWL-EVO1 as a Lung Cancer EVOC® Probe) has also opened sites in Manchester and London, with the ambition to recruit 25 patients and 25 healthy volunteers across all sites.
